Alpha Sophia for Health Insurers & Payors
Challenge


In 2026, health insurers and payors are navigating an increasingly complex environment defined by the rapid transition to value-based care and heightened regulatory oversight. Managing a provider network is no longer just about geographic coverage; it is about identifying high-value clinicians who can deliver superior outcomes while controlling the total cost of care. Without granular data on actual clinical performance, payors often struggle with "network bloat," where the sheer size of a provider list hides significant inefficiencies and variations in care quality.
Several structural inefficiencies frequently hinder the performance of insurance and payor organizations:
- The Outcome-Cost Paradox:Identifying HCPs who deliver optimal patient outcomes at a lower cost is nearly impossible using fragmented internal data. Without external benchmarking, insurers cannot see how their providers perform relative to the broader market, making it difficult to identify market gaps using healthcare market research.
- Data Silos and Integration Friction:Payors often maintain separate systems for claims, credentialing, and network management. This fragmentation leads to a "lagging view" of provider behavior, where network decisions are based on data that is months or years old, failing to reflect current practice patterns.
- Regulatory and Compliance Pressure:As the 2026 diagnostic landscape shifts, insurers face increased scrutiny regarding network adequacy and transparency. Failure to maintain an accurate, high-performing network can lead to significant penalties and member dissatisfaction.
- Difficulty Scaling Value-Based Contracts:Many payors struggle to move beyond small-scale pilots for alternative payment models. To scale, they need to identify which provider groups have the clinical capacity and patient volume to actually succeed in a risk-bearing environment, which requires a deeper look into healthcare market insights that drive smarter decisions.
Solution
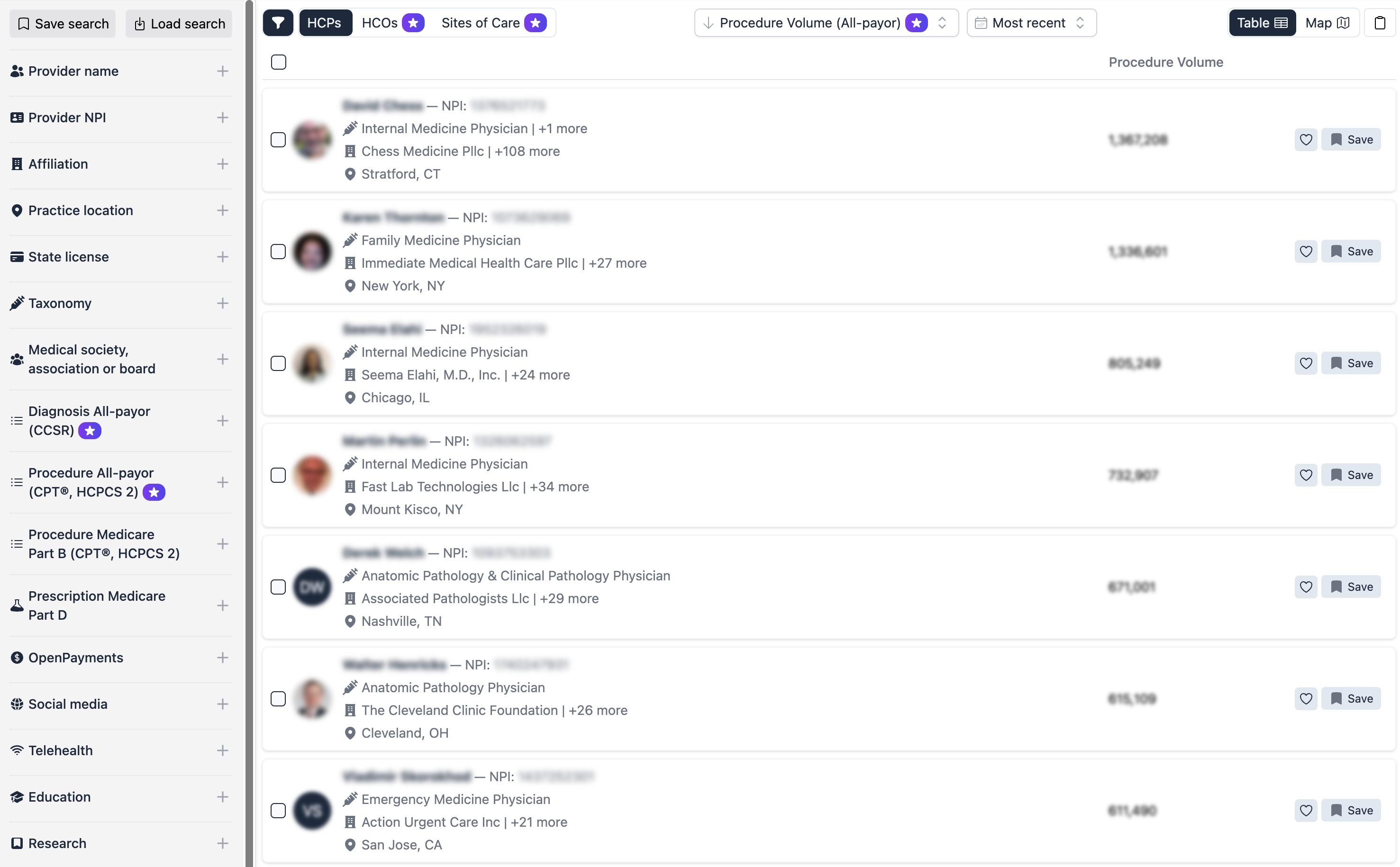

Alpha Sophia provides health insurers and payors with a robust, data-driven platform designed to optimize provider network management. By providing a single "Source of Truth" for physician-level billing, procedure volumes, and affiliations, Alpha Sophia enables payors to move from reactive administration to proactive network engineering.
With Alpha Sophia, payors can:
- Benchmark Provider Performance:Use all-payer claims data to compare your network providers against regional and national benchmarks. This allows you to identify high-performing clinicians and prioritize them for preferred status or value-based contracting.
- Improve Network Adequacy:Use advanced filters to map where care is actually happening. By analyzing real-world HCP data trends, you can pinpoint geographic or specialty gaps in your network and recruit the right providers to fill them.
- Streamline Provider Data Management:Access an accessible healthcare provider API that provides real-time updates on provider affiliations, locations, and specialties, ensuring your member-facing directories are accurate and compliant.
- Navigate Market Access and Pricing:Use clinical intelligence to inform your reimbursement strategies. By understanding the role of market access in drug pricing, payors can align their formularies and fee schedules with real-world clinical necessity.
Example
A regional Medicare Advantage plan looking to launch a specialized Chronic Care Management program for diabetic patients can use Alpha Sophia to identify the top 5% of endocrinologists and primary care physicians who: 1) Manage the highest volume of complex diabetic patients, 2) Demonstrate high adherence to preventive screening procedures, and 3) Are currently independent or part of groups ready for risk-sharing. By focusing recruitment on this high-performing cohort, the plan can ensure its new network delivers immediate value and lowers hospitalization rates by 25% within the first year.